Geneva, Tuesday 31 March 2020
The Thai-Cambodian border, 1988. The International Committee of the Red Cross ran a surgical hospital in one of the sprawling camps that were home to over 500,000 Cambodian refugees. The population that the hospital served included the refugees and anyone coming from inside Cambodia brave enough to navigate their way through the border minefields. (About 15% of our patients were mine-injured.) The hospital ran like clock-work under the all-seeing eye and disciplined but compassionate rule of the Head Nurse. Within twenty four hours there, I realised that she was the star of the show.
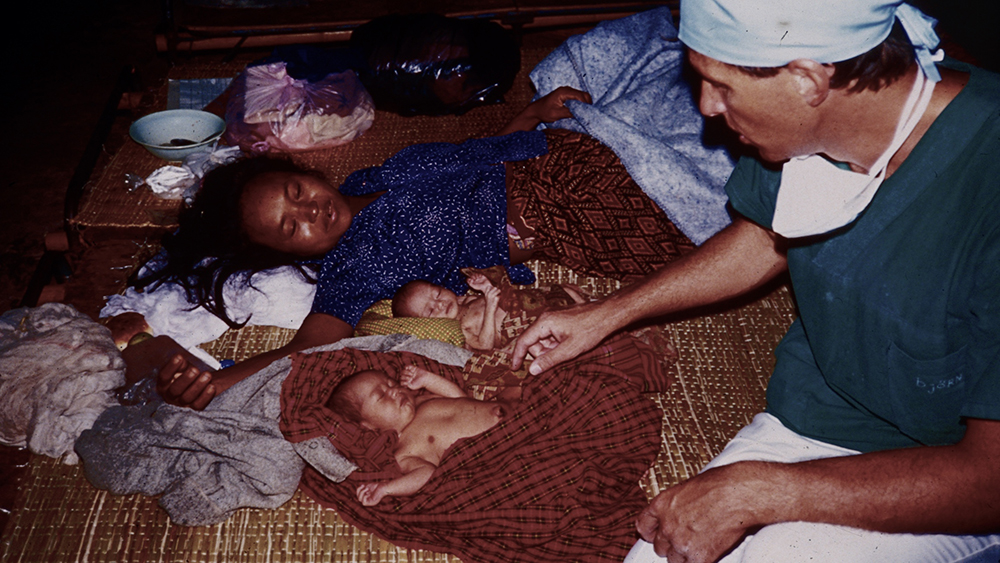
It was an extraordinary experience for a young surgeon! When on duty, it was for all-comers. Anything surgical arrived at the door. There was no specialist referral. Médecins Sans Frontières ran the maternity service next door. Many of their clients came from over the border after two or three days in labour. If the MSF midwife asked us to do a caesarian section – a daily event- there was no need for discussion. There was no possibility of an ultrasound scan. As a result, we would never know if the be-laboured woman was carrying twins until, having delivered one slippery little screamer, I exclaimed to the team “Wait a minute, there’s another one in here!” They never, ever believed me until I held up the evidence. I often wonder how often these days an obstetrician would undertake a caesarian section not knowing it was for twins.
Given seven years of field surgery, a glass or two of wine and a captive audience, I would happily tell surgical stories until the end of lockdown. But, I’ll stop here. There is a much more important COVID-19 story for repetition long after lockdown. It is the everyday and seemingly mundane story of running a hospital wherever it is. The provision of safe and effective curative medicine and surgery is dependent on a whole team of health-care professionals. They, in turn, are dependent on infrastructure including the equipment, machines, medicines, instruments, sterilisers, cleaners … the list is long. This infrastructure is held together by administrators responsible for recruiting and paying the staff, purchasing and putting in place the infrastructure, ensuring a constant supply of electricity and water, a functioning and dignified mortuary, drains that drain, disposal of medical waste … another long list. You get the picture? The COVID-19 pandemic has rightly elevated health-care workers to a position in public perception of being necessary for national integrity. This position, up to now, has been the near-exclusive domain of the armed forces. (This does not excuse constant use of terms like “war,” “battle” “frontline” “weapons” and “heroes.”) Let’s be clear though, the fuel of this engine is neither clever medicine nor swashbuckling surgery; it is the care provided by all the professionals concerned and, in particular, nursing care. Whilst health care is impossible without infrastructure, without care, it doesn’t even resemble health care. Go nurses! If during the next days and weeks, I drop other surgical stories into the Lockdown Diary, please bear this in mind.
The putting competition….. Yesterday I won 2 up; today 1 up. The running total is: 9 games to 4 in my favour. For those who have witnessed my wife’s putting for real on the course, this is most unexpected. But, if we believe the epidemiologists, there’s still a long way to go!
So, a moth goes in to see a dermatologist. “Hello” says the dermatologist. “What can I do for you?” The moth replies “Well, doctor, I’ve been feeling a bit down. I’ve lost my job. I’ve split up with my girlfriend. I’m maybe drinking a bit too much. Life’s a bit of drag, really.” The dermatologist says “I’m sorry to hear about all that. But I’m a dermatologist. I do skins. Maybe you should see a psychiatrist. Why did you come in here?” The moth says “Well, your light was on!”

I’m so enjoying your blog Robin
And I love your stories, so keep them coming
Gareth is working in General practice all be via a screen and a telephone with the occasional face to face contact
I’ve registered to return to the NHS
We are well and strong the house is so clean and the garden is manicured , dam I’ll have to get started on video editing that I’ve been meaning to do for the past 10 years!
Joke for you
Friend asked her friend. ” where your husband? ”
Friend answers. ” he’s in the garden”
Friend answers ” oh I’ve just been out there I didn’t see him ”
Friend answers ” you just need to dig a little ”
Enjoy your day and your putting
Bug hugs sent
Patricia xx
Très belle photo. La main de la maman accrochée à la couverture. La vôtre proche des bébés. Ce moment a dû s’inscrire en vous tous.
J’ai aussi des jumeaux, dont un sauvé par un chirurgien. Je connais la valeur des gestes qui soignent, d’où qu’ils proviennent. J’ai une tendresse immense pour toutes ces infirmières qui adoucissent tous ces moments difficiles.
Et une reconnaissance envers le chirurgien et son équipe qui ont permis à mon fils d’avoir 17 ans aujourd’hui.